GENERAL DENTAL SERVICES
TOOTH CONTOURING AND RESHAPING
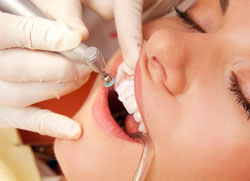
| Tooth reshaping and contouring is a procedure to correct crooked teeth, chipped or irregularly shaped teeth or even overlapping teeth in a single session. This is commonly used to alter the length, shape or position of your teeth, correct small problems with bite. It is common for bonding to be combined with tooth reshaping.
This procedure is ideal for candidates with normal, healthy teeth but who want subtle changes to their smile. We will take xrays to evaluate the size and location of the pulp of each tooth to ensure that theres enough bone between the teeth to support them. |
 |
BLEACHING
(TOOTH WHITENING)
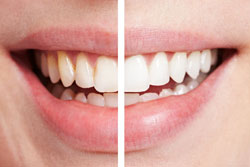
Bleaching is a common and popular chemical process used to lighten teeth. Some people get their teeth bleached to make stains disappear, while other just want a brighter smile. Discoloration occurs in the enamel and can be caused by medication, coffee, tea, and cigarettes. Discoloration also can be
hereditary (genetic makeup) or due simply to getting older.
 |
Bleaching can be performed in the office or, under dental supervision, at home. Many patients enjoy bleaching at home because it is more convenient. Treatment begins when the dentist creates a custom mouthpiece to ensure the correct amount of whitening solution is used and that your teeth are properly exposed. Typically, whitening at home takes 10-14 days, and sometimes more, depending on the desired shade you wish to
achieve. Whitening in the office may call for one or more 45-minute to one-hour visits to your dentists office. |
TOOTH COLORED FILLINGS/COMPOSITES
A composite filling is a tooth-colored plastic and glass mixture used to restore decayed teeth. Composites are also used for cosmetic improvements of the smile by changing the color of the teeth or reshaping disfigured teeth. Bonding lasts several years and often requires only a single office visit. Bonding is more susceptible to staining or chipping than other forms of restorations. When teeth are chipped or slightly decayed, bonded composite resins may be the material of choice. Bonding also is used to fill small cavities, to close spaces between teeth or to cover the entire outside surface of a tooth. Sometimes after receiving the composite, the patient may experience postoperative sensitivity that lasts for few days.
VENEERS
|
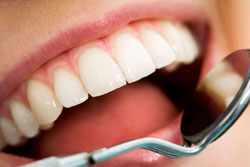
Veneers are ultra-thin shells of ceramic(porcelain) or a composite resin material, which are bonded to the front teeth. This procedure requires little or no anesthesia and can be the ideal choice for improving the appearance of the front teeth. Veneers are placed to mask discolorations, to brighten teeth and to improve a smile.
Veneers are an excellent alternative to crowns in many situations. They provide a much more conservative approach to changing a tooths color, stained by tetracycline. Patients with gaps between their front teeth or teeth that are chipped or worn may consider veneers. Generally, veneers will last for many years, and the technique has shown remarkable longevity when properly performed.
|
 |
DENTAL CROWNS/CAPS
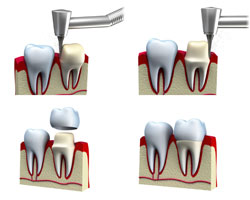
A crown is a restoration that covers or caps a tooth to restore it to its normal shape and size, strengthening and improving the appearance of a tooth. Crowns are necessary when a tooth is generally broken down and fillings wont solve the problem. If a tooth is cracked, a crown holds the tooth together to seal the cracks so the damage does not get worse. Crowns are also used to restore a tooth when there is not enough of the tooth remaining to provide support for a large filling, attach a bridge, protect weak teeth from fracturing, restore fractured teeth or cover badly shaped or discolored teeth.
| To prepare the tooth for a crown, it is reduced so the crown can fit over it. An impression of the teeth and gums is made and sent to the lab for the crown fabrication. A temporary crown is fitted over the tooth until the permanent crown is made. On the next visit, the temporary crown is removed and the permanent crown is fitted and cemented onto the tooth.
Crowns should last approximately 5 to 10 years. However, with good oral hygiene and supervision, most crowns will last for a much longer period of time. Some damaging habits like grinding your teeth, chewing ice or fingernail biting may cause this period of time to decrease significantly.
|
 |
PORCELAIN DENTAL BRIDGE
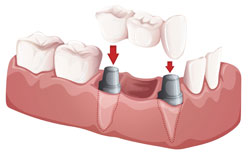 |
A bridge is a fixed dental restoration used to replace a missing tooth by joining an artificial tooth permanently to adjacent teeth. A bridge is fabricated by reducing the teeth on either side of the missing tooth or teeth by preparation pattern determined by the location of the teeth and by the material from which the bridge is fabricated. In other words, the abutment teeth are reduced in size to accommodate the material to be used to restore the size and shape of the original teeth in a correct alignment and contact with the opposing teeth. The materials used for the bridges include gold, porcelain fused to metal or in the correct situation porcelain alone. Getting a bridge usually takes two or more visits. |
TYPES OF BRIDGES:
CONVENTIONAL FIXED DENTAL BRIDGE:
For this bridge, the dentist trims both teeth adjacent to the missing tooth, and cements a porcelain crown on top of each. Attached to the two crowns is an artificial tooth(or pontic) in the middle. This arrangement provides maximum support since any force applied to the artificial tooth is spread to the two nearby sound teeth.
CANTILEVER BRIDGE:
Only one adjacent tooth is trimmed and fitted with a crown that is attached to the artificial tooth. Trimming a tooth involves removing large amounts of tooth structure from healthy teeth, so a dentist might choose this option to preserve tooth structure. The downside for cantilever bridges is that support for the artificial tooth is provided by only the one tooth. This limits its use to areas of the mouth which receive little stress during chewing.
RESIN BONDED BRIDGE OR MARYLAND BRIDGE
These bridges require minimal trimming of adjacent teeth, and rely on plastic resin to hold the artificial tooth in place. This makes them very weak, and should therefore only be considered for replacing front teeth, provided that the gums are healthy and the surrounding teeth do not have extensive dental fillings.
DENTAL INLAYS AND ONLAYS
Inlays and onlays are indirect dental restorations that are fabricated by the dental laboratory that offer a well-fitting, stronger, longer lasting reparative solution to tooth decay or similar damage. They are conservative alternative to full coverage dental crowns. These restorations are beneficial from both an esthetic and functional point of view.
| Typically, an inlay or onlay procedure is completed in two dental visits. During the first visit, the dentist prepare the damaged tooth. A molded impression of the tooth is then taken and sent to a dental laboratory, where an inlay or onlay is fabricated. This can either be made from gold, porcelain or resin materials. A fitted, provisional inlay/onlay in the shape of the final restoration can be created during this visit to protect the tooth while the final restoration is being fabricated. |
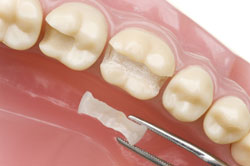 |
During the second visit, the provisional temporary is removed and the inlay/onlay is placed. Once fitted the inlay or onlay is bonded onto the tooth and the margins are polished.
DENTURES
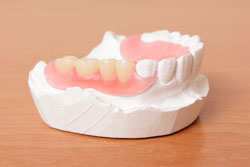 |
A denture is a removable replacement for missing teeth and adjoining tissues. Complete dentures replace all of the teeth, while a partial denture fills in the spaces created by missing teeth and prevents other teeth from shifting position. Complete dentures are either conventional or immediate. A conventional denture is placed in the mouth after all of the teeth have been removed and the extraction sites have healed. An immediate denture is placed as soon as the teeth are removed. Partial dentures are either flexible, acrylic, cast or combination of cast/flexible. |
- Who needs a denture?
Candidates for complete dentures have lost most or all of their teeth. A partial denture is suitable for those who have some natural teeth remaining. A denture improved chewing ability and speech, and provides support for facial muscles. A denture can greatly enhance a patients facial appearance and smile.
- How do you get a denture?
The denture process takes about one month. There are usually five or more appointments needed to complete the process. The process includes the initial diagnosis; the making of an impression and wax bite to determine the dimensions and proper jaw position; a try-in to assure proper color, shape and fit; placement of the final denture; and any minor adjustments. New denture wearers need time to get accustomed to their new teeth, because even the best-fitting dentures will feel awkward at first. Your normal speaking ability usually resumes shortly after final denture placement. In addition, in order to become accustomed to chewing with the new denture, it is often recommended that you start with soft, easy to chew foods.
- Are there any alternatives to dentures?
Dentures are no longer the only way to restore a mouth that has little or no teeth. Dental implants are artificial tooth roots that are surgically anchored into your jaw to hold a replacement tooth or bridge in place. Implants and bridges may more closely resemble the feel of real teeth.
Care for the Dentures:
- Remove and brush the denture daily, preferably with a brush designed specifically for cleaning dentures, using a denture cleanser.
- Never use harsh, abrasive cleansers, including toothpastes, because they may scratch the surface of the denture, leaving it susceptible to plaque and stains.
- Do not sterilize your denture with boiling water because it will cause it to become warped.
- If you wear a partial denture, be sure to remove it before brushing your natural teeth.
- It is considered best to remove your denture at night. It allows the gum tissue to rest and allows normal stimulation and cleansing by the tongue and saliva. When not in use, you should soak your dentures in water. Get in the habit of keeping the denture in the same safe and handy place to reduce the likelihood of misplacing it.
TREATMENT OF GUM
DISEASE (PERIODONTICS)
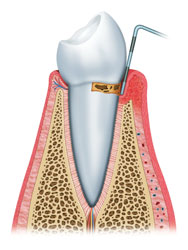
| Gum disease, or periodontal disease is a chronic inflammation and infection of the gums and surrounding tissue. It is the major cause of about 70 percent of adult tooth loss, affecting three out of four persons at some point in their life. Periodontal diseases include gingivitis and periodontitis. In the early stages of gum disease, most treatment involves a special cleaning called scaling and root planning, which removes plaque and tartar around the tooth and smoothing the root surfaces. Antibiotics or antimicrobials may be used to supplement the effects of scaling and root planning. If the general dentist believes that the gum disease requires treatment by the specialist, the patient will be referred to a specialist. |
 |
Causes of gum disease:
Bacterial plaque- a sticky, colorless film that constantly forms on the teeth-is recognized as the primary cause of gum disease. If plaque isnt removed each day by brushing, flossing and rinsing, it hardens into a rough, porous substance called calculus(also known as tartar). Toxins produced and released by bacteria in plaque irritate the gums. These toxins cause the breakdown of fibers that hold the gums tightly to the teeth, creating periodontal pockets that fill with even more toxins and bacteria. As the disease progresses, pockets extend deeper, and the bacteria moves down until the bone that holds the tooth in place is destroyed. The tooth eventually will fall out or require extraction.
Other factors of gum disease:
- Genetics
- Smokers and spit tobacco users
- Leukemia, AIDS, uncontrolled diabetes
- Pregnant women
Signs of gum disease:
- Red, swollen, tender gums
- Bleeding while brushing or flossing
- Gums that pull away from teeth
- Pus between the gum and tooth
- Persistent bad
breath (halitosis)
- Change in the way the teeth fit together when the patient bites
ROOT CANAL
THERAPY (ENDODONTICS)
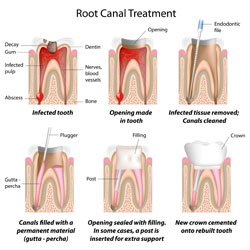
| Root canal therapy is a procedure that removes the damaged pulp tissue. Damaged pulp causes increased blood flow and activity in the tooths cells. Pressure may build up within a tooth that cannot be relieved, causing pain that is commonly left when biting down, chewing or consuming hot or cold foods and drinks. Without treatment the infection will spread and bone around the tooth will begin to degenerate and pain usually worsens. If your general dentist recommends root canal, he or she will perform the treatment or refer you for treatment to an endodontist, which is a specialist who treats injuries,
diseases, and infections of the tooth pulp. |
 |
Procedure:
A space in created into the tooths pulp chamber, which, along with any infected root canal, is cleaned of all diseased pulp and reshaped. Medication may be inserted into the area to fight bacteria. Depending on the condition of the tooth, the crown may then be sealed temporarily to guard against recontamination or the dentist may immediately fill the canals.
Temporary fillings are removed and the pulp chamber and canals are filled on the next visit. If the tooth is still weak, a post may be inserted above the canal filling to help rebuild the tooth. Once filled the area is permanently sealed. Finally, a crown is normally placed over the tooth to strengthen its structure and improve its appearance.
Post-op Root canal therapy:
There may be some inflammation around the gum tissues, which may cause discomfort for few days. This can be controlled by an over-the-counter pain reliever. A follow-up visit to your dentist will help him or her review how the tissue is healing. From this point on, brush and floss regularly, avoid chewing hard foods on the treated tooth, and see your dentist on a regular basis for cleanings and examination.
Options to root canal therapy:
The only alternative to root canal therapy is to extract the tooth; however,this alone can cause the surrounding teeth to move, resulting in a bad bite. Though a simple extraction may be perceived as less expensive, the empty space left behind will require an implant or a bridge, which ultimately can be more costly than root canal
therapy
MOUTHGUARDS
 |
An athletic mouth guard, also called as mouth protector is a flexible appliance that is worn during athletic and recreational activities to protect teeth from trauma, Custom-fabricated mouth guards are essential for preventing athletic oral/facial injuries, such as broken teeth, jaw fractures, cerebral hemorrhages, and neck injuries. Mouth protectors usually cover the upper teeth and protect the oral soft tissues. It is an essential piece of athletic gear that should be part of the standard equipment from an early age. In fact, studies show that athletes are 60 times more likely to suffer harm to the teeth if they are not wearing a mouth guard. |
Types of
Mouthguards:
- Custom-fitted: These are made by your dentist for you personally They are more expensive than the other versions, but because they are customized, usually offer the best fit.
- Stock: These are inexpensive and come preformed, ready to wear. Unfortunately, they often dont fit very well. They can be bulky and can make breathing and talking difficult.
- Boil and bite: These mouth protectors can be bought at many sporting goods stores and drugstores and may offer a better fit than stock mouth guards. They are first softened in water(boiled), then inserted and allowed to adapt to the shape of your mouth.
If you have a retainer or other removable appliances, do not wear the mouth guard during any contact
sports
NIGHTGUARD (OCCLUSAL SPLINT)
Bruxism is the technical term for grinding and clenching of the teeth that may cause facial pain. People who grind and clench their teeth, called bruxers, unintentionally bite down too hard at inappropriate times, such as in their sleep. In addition to grinding teeth, bruxers also may bite their fingernails, pencils and chew the inside of their cheeks.
People usually arent diagnosed with bruxism until it is too late, as many people dont realize they have the habit. People who have otherwise healthy teeth and gums can clench so often and so hard that over time their teeth become sensitive. They experience jaw pain, tense muscles and headaches along with excessive wear on their teeth.
Bruxism is triggered by people with certain types of personalities. They may have a nervous tension and a hard time handling stress. Anger, pain, and frustration can cause people to start showing the beginning signs of bruxism without them even knowing it. People who are aggressive, competitive and hurried also may be at a greater risk for
bruxism.
Patient may present with a variety of symptoms:
- Anxiety, stress and tension
- Depression
- Earache
- Eating
disorders
- Headaches, migraines,tinnitus
- Loose teeth, gum recession
- Neck pain
- Insomnia
- Sore or painful jaw
What can be done? The dentist automatically checks for physical signs of bruxism and if it seems to be present the condition may be observed over several visits before recommending and starting therapy. The objective of therapy is to get the bruxer to change behavior by learning how to rest the tongue, teeth and lips properly. When some people become aware of their problem, simply advising them to rest their tongue upward with teeth apart and lips shut may be enough to change their behavior and relieve discomfort.
| Night guards
(dental guards or occlusal splints) can be worn by bruxers to absorb the force of biting. This appliance can prevent future damage to the teeth and helps reduce muscle strain by allowing the upper and lower jaw to move easily with respect to each other. Night guards are typically made of plastic and fit over some or all of upper and/or lower teeth. |
 |
Treatment goals include:
- Constraining the bruxing pattern to avoid damage to the temporomandibular joints
- Stabilization of occlusion(bite)by minimizing gradual changes to the position of the teeth
- Preventing tooth damage
- Revealing the extent and patterns of bruxism through examination of the markings on the splints surface.
If teeth grinding is due to stress, a bruxer may be able to prevent the problem with counseling or strategies that promote relaxation, such as exercise and meditation. Biofeedback is used to treat daytime clenchers by using an electronic device to measure muscle activity and to teach patients how to reduce muscle activity when the biting force becomes too great.
TOOTH EXTRACTIONS
A tooth that is severely damaged may need to be removed. The general dentist will evaluate, diagnose and if the tooth is indicated for extraction, he or she will extract the tooth or refer the patient to the oral surgeon. The dentist will give you a local anesthetic numb the area where the tooth will be removed. After the tooth is removed, you may need stitches. Some stitches dissolve over time, and some have to be removed after a few days. Your dentist will tell you whether your stitches need to be removed. You can gently bite down on a cotton guaze pad placed over the extraction site. After the extraction, you will be advise of post-op care and regimen.
Post-operative Care after tooth extraction:
- Take painkillers as prescribed by your dentist or oral surgeon.
- After 24 hours, rinse your mouth gently with warm salt water several times a day to reduce swelling and relieve pain. Make your own salt water by mixing 1 teaspoon of salt in a 8-oz glass of warm water.
- Change gauze pads before they become soaked with blood.
- Relax after surgery. Physical activity may increase bleeding.
- Avoid smoking.
- Eat soft foods, such as gelatin, pudding, or thin soup. Gradually add solid foods to your diet as healing progresses.
- Do not lie flat. This may prolong bleeding. Prop up your head with pillows.
- Avoid rubbing the area with your tongue.
- Continue to carefully brush your teeth and tongue
|